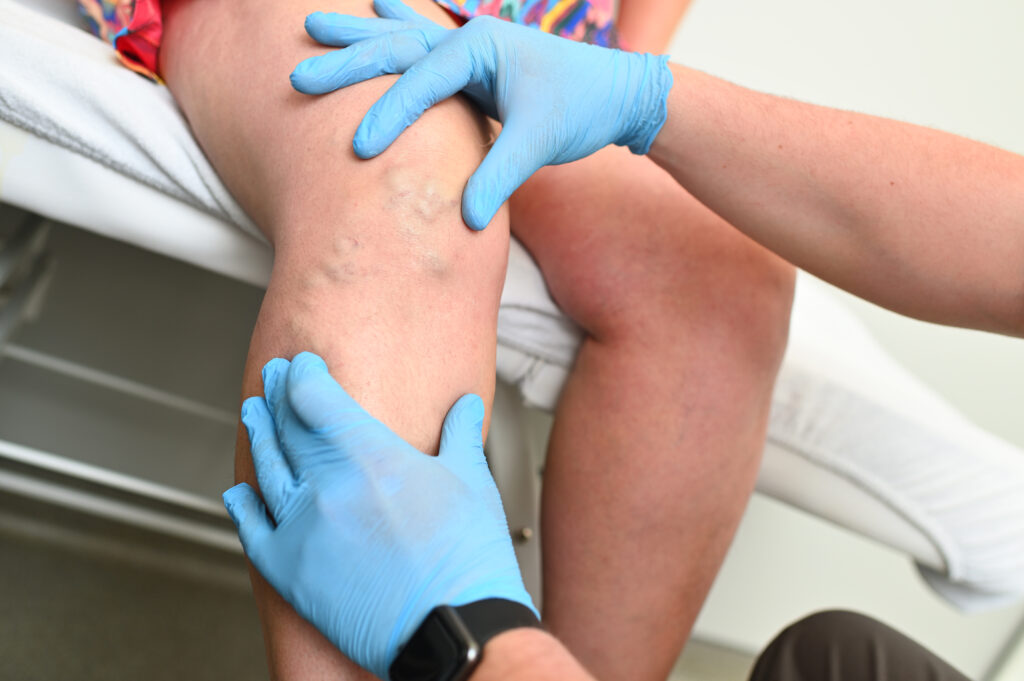
If you have noticed that the veins on your legs look more prominent than they did a few years ago, or that what started as a minor ache after a long day has turned into a persistent, heavy feeling, you are not imagining it. Varicose veins are a progressive condition – left unaddressed, they tend to worsen gradually over months and years. Understanding why this happens and recognising the early warning signs are the first steps toward doing something about it.
This article explains the mechanics behind varicose vein progression, the lifestyle and biological factors that speed things up, and what options are available to Sunshine Coast residents who want to get ahead of the problem.
How Varicose Veins Form in the First Place
To understand why varicose veins get worse, it helps to understand how they develop. The veins in your legs are responsible for returning blood to the heart – a considerable task given that blood must travel upward against gravity. Inside these veins are tiny one-way valves that open to allow blood to flow upward, then close quickly to stop it from flowing back down.
When these valves weaken or are damaged, they can no longer close properly. Blood begins to flow backward and pool in the lower sections of the vein. This pooling increases pressure on the vein wall, causing it to stretch, bulge, and twist. The result is what we recognise as a varicose vein.
Crucially, this is not a static process. Once a valve fails, the excess pressure it creates can place strain on the valves below it, causing a cascade effect. This is why a single small varicose vein can gradually multiply into a cluster, and why symptoms that were once mild can become more pronounced over time.
Why Varicose Veins Progress Over Time
Varicose veins rarely improve on their own. Without treatment, the underlying valve dysfunction continues, and the mechanical pressure on surrounding vein walls builds. Several factors influence how quickly this progression occurs.
Genetics and Family History
If one or both of your parents have varicose veins, your likelihood of developing them – and experiencing faster progression – is significantly higher. The structural integrity of vein walls and valve function has a strong inherited component. People with a family history of venous disease tend to develop varicose veins earlier in life and are more likely to see them worsen over time.
Prolonged Standing or Sitting
Occupations that require long hours on your feet – nursing, hospitality, retail, teaching – or desk jobs that involve extended periods of sitting both take a toll on venous circulation. When your legs are stationary for long stretches, the calf muscles cannot assist in pumping blood upward. Pressure builds inside the leg veins, adding strain to already-compromised valves and accelerating their deterioration.
Pregnancy
Pregnancy places considerable demand on the venous system. Blood volume increases significantly, and the growing uterus exerts direct pressure on the pelvic veins, slowing blood flow from the lower limbs. Oestrogen and progesterone also cause vein walls to relax and become more pliable, making them more susceptible to stretching. Varicose veins that appear during pregnancy may improve after delivery, but they do not always disappear – and each subsequent pregnancy can compound the issue.
Excess Body Weight
Carrying excess weight places additional pressure on the circulatory system, particularly in the lower limbs. This increases the workload on vein valves and can hasten the weakening of vein walls. A more sedentary lifestyle often accompanying excess weight further reduces the effectiveness of the calf muscle pump, compounding the problem.
Age and Hormonal Changes
As we age, vein walls naturally lose some of their elasticity and the valves become less efficient. This is a normal part of ageing, but it means that people who already have early-stage varicose veins in their thirties or forties are likely to notice more significant symptoms by their fifties and sixties. Hormonal changes associated with menopause can also contribute to further valve weakening.
Smoking
Substances inhaled through smoking can damage vein walls and impair overall circulation. This cumulative effect can cause varicose veins to worsen more rapidly and also reduces the body’s ability to recover from minor venous injury.
Warning Signs That Your Varicose Veins Are Progressing
Many people dismiss varicose veins as a cosmetic concern – and in the early stages, they may be nothing more than that. But the condition exists on a spectrum, and certain signs suggest the underlying venous insufficiency is advancing.
Warning signs worth taking seriously include:
- Aching, heaviness, or fatigue in the legs, particularly after standing or at the end of the day
- Swelling around the ankles or lower legs, especially in warmer weather
- Itching or burning skin over the affected vein
- Skin discolouration – a brownish or reddish tinge near the ankle or lower leg
- Hardening or thickening of the skin in the lower leg
- Development of new spider veins alongside existing varicose veins
- Cramping or restless legs at night
- Any open or slow-healing sore near the ankle
If you are noticing skin changes or developing sores, this is a sign that the condition has moved beyond early-stage and is approaching or already at a stage where complications become more likely.
Potential Complications of Untreated Varicose Veins
Left to progress without assessment or management, varicose veins can lead to a range of complications:
Superficial Thrombophlebitis
Blood that pools and becomes stagnant in a varicose vein can clot. This is known as superficial thrombophlebitis – the vein becomes inflamed, painful, red, and tender to the touch. While it is typically not life-threatening, it is uncomfortable and signals that venous disease is progressing.
Venous Eczema and Skin Changes
Sustained high pressure in the leg veins can cause fluid to leak into surrounding tissue, leading to persistent swelling. Over time, this results in skin changes – discolouration, thickening, and fragility. The skin becomes prone to breaking down, and minor knocks or scratches can open into wounds that are slow to heal.
Venous Leg Ulcers
Venous leg ulcers are one of the more serious consequences of long-standing venous insufficiency, occurring in up to 20 per cent of people with advanced varicose vein disease. These are open sores, typically near the ankle, that are difficult to heal and prone to infection. They significantly affect quality of life and can require lengthy treatment. Addressing the underlying venous problem early is the most effective way to reduce the risk of ulcers developing.
Bleeding
Varicose veins that sit close to the skin surface are vulnerable to bleeding from even minor trauma – sometimes simply from a graze or a nick while shaving. In elderly patients with fragile skin, this can produce alarming bleeding that is difficult to control without direct pressure. While serious haemorrhage is rare, it is a preventable risk that underscores the value of early treatment.
The Relationship Between Varicose Veins and Spider Veins
Spider veins are often mistakenly thought of as simply a cosmetic nuisance separate from varicose veins. In reality, they frequently share the same underlying cause – venous reflux and elevated pressure in the superficial venous system. Spider veins that appear alongside existing varicose veins can be a sign that venous pressure is increasing and spreading to smaller vessels. Treating both the underlying venous insufficiency and the visible surface vessels tends to produce the most thorough and lasting results.
What You Can Do Early
The good news is that early-stage varicose veins can often be managed effectively, and the complications described above are largely preventable with appropriate assessment and care.
Lifestyle Modifications
While lifestyle changes cannot reverse existing varicose veins, they can slow progression and reduce symptoms. Useful steps include:
- Taking regular movement breaks if you sit or stand for extended periods
- Elevating your legs above heart level for 15 minutes several times a day
- Wearing graduated compression stockings during the day
- Maintaining a healthy weight to reduce venous pressure
- Staying active – walking and swimming are particularly supportive of venous return
- Avoiding prolonged exposure to heat, which causes veins to dilate and can worsen symptoms
These measures can ease discomfort and slow the worsening of existing veins, but they are management strategies, not treatments. They do not address the underlying valve dysfunction.
Getting a Proper Assessment
Many people delay seeking assessment because they assume varicose veins are purely cosmetic, or because they are waiting until symptoms become unbearable. The reality is that earlier assessment typically means simpler and more effective treatment options. By the time complications develop, treatment becomes more complex and recovery more involved.
A thorough initial assessment for varicose veins should always include a colour duplex ultrasound scan. This non-invasive scan maps the venous system in your legs, identifies which valves are failing, and traces where venous reflux is occurring. Without this detailed picture, it is not possible to plan appropriate treatment.
H2: Modern Varicose Vein Treatment Options on the Sunshine Coast
Sunshine Vein & Cosmetic Clinic, we offer a range of minimally invasive, non-surgical treatment options for varicose veins that do not require hospitalisation or general anaesthesia. Most patients can return to their normal activities within a day or two. Our treatments for Sunshine Coast varicose veins include:
Endovenous Laser Ablation (EVLA)
EVLA is the most commonly used primary treatment for varicose veins caused by valve failure in the great or small saphenous veins. A fine laser fibre is guided into the affected vein under ultrasound guidance. Laser energy is then delivered along the length of the vein, causing it to close. The vein is gradually absorbed by the body, and blood flow is redirected through healthy vessels. This Sunshine Coast varicose vein laser treatment is performed under local anaesthetic in-clinic and has a significantly lower recurrence rate than traditional surgical stripping.
Ultrasound-Guided Foam Sclerotherapy (UGS)
Foam sclerotherapy involves injecting a pharmaceutical foam directly into the varicose vein under ultrasound guidance. The foam displaces blood within the vein and irritates the vessel wall, causing it to close. This approach is used for varicose veins of various sizes and is often performed as an adjunct to EVLA to treat the branches that feed off the main faulty vessel.
Medical Superglue (VenaBlock)
This technique uses a medical-grade adhesive to seal the affected vein from within. The superglue is injected through a small catheter under ultrasound guidance, and the vein collapses and is then absorbed by the body. It is a suitable option for certain patients and is performed without the need for tumescent anaesthesia or compression stockings post-procedure.
Microsclerotherapy and Sclerotherapy for Spider Veins
For patients with spider veins or smaller surface vessels alongside varicose veins, microsclerotherapy – injecting a very fine sclerosant solution directly into the visible vessels – is typically used once the underlying varicose veins have been treated. Addressing the root cause first produces far better cosmetic outcomes than treating spider veins alone.
Ambulatory Phlebectomy
For bulging varicose veins that sit close to the skin surface, ambulatory phlebectomy involves the physical removal of the vein through very small incisions. This is performed under local anaesthetic and is often combined with EVLA for larger varicose vein clusters.
When to Seek Assessment
There is no need to wait until varicose veins become unbearable before seeking an opinion. Consider booking an assessment if:
- You can see bulging, rope-like veins on your legs
- You experience persistent leg aching, heaviness, or swelling
- Your symptoms are worsening over months
- You have noticed skin changes near your ankles or lower legs
- You have a strong family history of varicose veins and want to understand your current vein health
- You are planning a pregnancy and want baseline information about your venous system
Early assessment costs little and provides a clear picture of what is happening beneath the surface. It also means that if treatment is needed, the options available to you are likely to be simpler and less intensive than they would be if you wait.
Varicose Vein Assessment and Treatment on the Sunshine Coast
Sunshine Vein & Cosmetic Clinic is led by Dr Hugo Pin, a physician with extensive specialist experience in vein assessment and treatment. The clinic is located in Minyama, on the Sunshine Coast, and offers comprehensive duplex ultrasound scanning alongside a full range of minimally invasive Sunshine Coast varicose vein removal and treatment options – all in a single, accessible location.
Whether you are in the early stages of noticing visible veins or are already dealing with ongoing symptoms, an assessment with our team is the first step toward understanding what is happening and what can be done. To learn more or to arrange a consultation, visit our vein procedures page or contact the clinic directly.
Disclaimer: This article is intended for general informational purposes and does not substitute for professional medical advice, diagnosis, or treatment. Vein conditions vary from person to person, and the treatment options that are appropriate for you will depend on your individual clinical assessment. If you have concerns about varicose veins or any other vein-related symptoms, please consult a qualified healthcare practitioner. Any invasive or minimally invasive procedure carries risks, and you should discuss these fully with your treating physician before proceeding.